Comprehensive Guide to Hand Amputation and Replantation Surgery: Treatment, Recovery, and Success Rates
If you face a severe hand injury, amputation and replantation surgery address traumatic loss of fingers or hands. At North Texas Hand Center, P.A., we provide expert care using advanced microsurgical techniques to restore circulation, function, and appearance when possible. This guide explains causes of amputations, the microsurgical methods we use in replantation, and the recovery process. Understanding these elements helps you and your family evaluate treatment options and rehabilitation pathways.
When an accident causes partial or complete amputation, timely surgical intervention can make a significant difference. We emphasize practical steps that influence outcomes: how the amputated part should be handled before arrival at a trauma center, how ischemia is minimized, and how coordinated perioperative care improves survival and function. Our goal is to help patients and caregivers make informed decisions while preserving options for the best possible recovery.
What Causes Hand and Finger Amputations? Understanding Injury Types and Trauma
Hand and finger amputations result from various traumatic injuries, each with distinct implications for treatment and recovery. Recognizing the injury type supports prevention and timely medical care.
Which Types of Hand Trauma Lead to Amputation?
Some hand injuries may require amputation, such as:
- Severe Fractures: Complex fractures that cannot be repaired may lead to amputation.
- Lacerations: Deep cuts that sever nerves, blood vessels, or tendons can result in the loss of fingers or hands.
- Crushing Injuries: Injuries from heavy machinery or accidents can cause irreparable damage to the hand structure.
These injuries demand prompt medical assessment to determine the viability of the amputated part and the optimal treatment approach.
In the immediate aftermath of an injury, practical triage steps can affect replantation options. Preserve an amputated digit by gently rinsing visible contaminants with clean water, wrapping it in sterile gauze or a clean cloth, placing the wrapped part in a waterproof bag, and then placing that bag on ice—not directly on ice—to reduce tissue temperature and slow cellular damage. Avoid immersion in water or any harsh chemicals and do not wrap the amputated part in dry ice or put it in direct contact with ice. Transport time and the way the part is protected influence ischemia duration and surgical options.
How Does Hand Anatomy Influence Amputation Severity?
The severity of an amputation is shaped by hand anatomy. Important factors include:
- Blood Supply: Adequate blood flow is essential for healing; injuries that compromise blood vessels can lead to more severe outcomes.
- Nerve and Tendon Involvement: Damage to nerves and tendons can affect the functionality of the hand, making reattachment more complex.
- Anatomical Variations: Individual differences in hand structure can impact surgical decisions and outcomes.
Our surgeons use these anatomical considerations to plan treatment and estimate recovery timelines.
Preoperative assessment typically includes clinical examination and imaging to define the level of bone loss, joint involvement, and condition of soft tissues. X-rays identify fracture patterns and joint integrity; ultrasound or angiography may help evaluate the vascular pedicle when available. Together, these findings guide whether reconstruction or primary amputation is the safer option and help our surgical team discuss realistic expectations with you and your family.
What Are the Microsurgical Techniques Used in Hand Replantation?
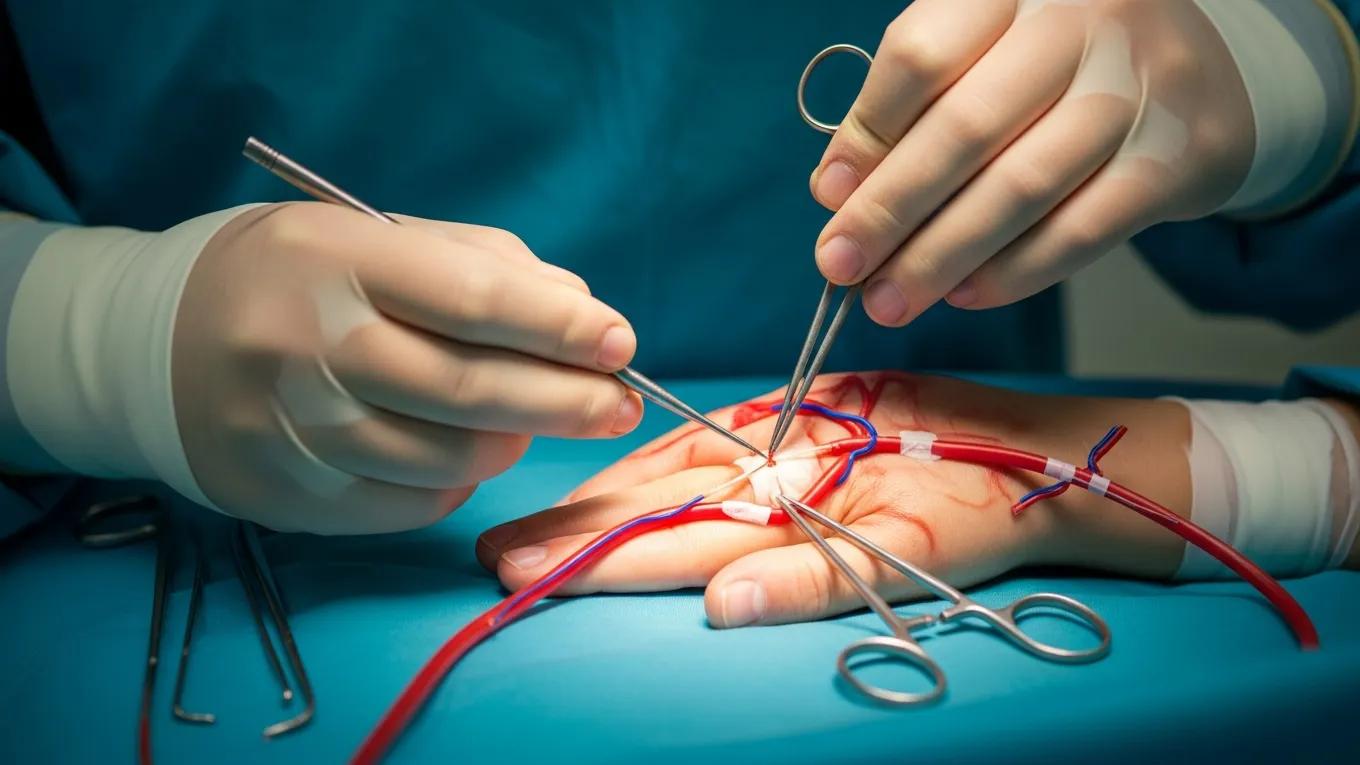
Microsurgery enables precise reconnection of severed nerves, blood vessels, bone, and soft tissues. These techniques are central to restoring circulation, sensation, strength, and appearance after traumatic amputations.
At North Texas Hand Center, P.A., we emphasize the comprehensive role of microsurgery in achieving successful replantation outcomes.
Over the past several decades, the development of microsurgery has enabled replantation of nearly all amputated parts, including distal phalanges and fingertips. Our primary goals are to re-establish blood flow and regain sufficient function and sensation. Management requires careful preoperative preparation, experienced microsurgical technique, and continuous postoperative care. Key factors that influence outcome include the type and level of injury, ischemia time, diabetes history, patient age and sex, and smoking status. During replantation, our surgeons typically perform bone stabilization, tendon repair, arterial and venous anastomoses, nerve coaptation, and skin coverage. You may want to learn more about what does a hand specialist doctor do.
Microsurgical replantation is multi-step and multidisciplinary. Key intraoperative components that typically follow one another are:
- Bone stabilization to restore length and alignment and provide a stable platform for soft-tissue repair.
- Tendon repair to re-establish active motion when possible and to balance flexor and extensor mechanisms.
- Arterial and venous anastomoses performed under magnification to restore inflow and outflow; venous repair is often as critical as arterial repair for preventing congestion.
- Nerve coaptation to permit sensory and motor reinnervation over time; where gaps exist, nerve grafting can be used.
- Skin coverage and soft-tissue reconstruction to protect repairs and provide durable coverage.
Other intraoperative strategies include temporary external fixation when contamination is present, staged debridement of nonviable tissue, and the use of local or regional flaps to replace missing soft tissue. Our experienced microsurgical team coordinates timing, sequence, and contingencies when parts are heavily damaged.
How Is Vascular Repair Performed During Replantation Surgery?
Vascular repair in replantation follows several essential steps:
- Identification of Blood Vessels: Our surgeons locate and prepare the severed blood vessels for reconnection.
- Vascular Anastomosis: Using microsurgical techniques, the blood vessels are meticulously sewn back together to restore blood flow.
- Monitoring Blood Flow: After repair, blood flow is monitored to ensure the success of the reattachment.
This precise vascular work is critical to the survival of the reattached part and requires specialized expertise.
Vascular repair often requires delicate handling to prevent thrombosis. Small-gauge sutures and microsurgical instruments are used to align vessel walls with minimal tension. Our surgeons may perform multiple venous repairs when possible because venous outflow is a common point of failure. Intraoperative use of heparinized saline irrigations, topical vasodilators, and systemic anticoagulation protocols are tailored to each case to reduce clot formation while balancing bleeding risk.
After revascularization, our team closely observes color, capillary refill, turgor, and temperature of the replanted part. When available, adjunct monitoring such as Doppler signals or implantable sensors can provide objective data on circulation in the immediate postoperative period.
What Role Does Nerve Repair Play in Functional Restoration?
Nerve repair is essential for restoring sensation and movement. Key considerations include:
- Techniques for Nerve Repair: Our surgeons may use direct suturing or nerve grafts to reconnect severed nerves.
- Impact on Functional Recovery: Successful nerve repair can significantly enhance the functional outcomes of replantation.
- Long-term Outcomes: Patients may experience varying degrees of recovery, depending on the extent of nerve damage and the success of the repair.
Successful nerve repair is an important determinant of long-term hand function and patient satisfaction.
Recovery of sensation and motor control is gradual. Early sensory re-education, desensitization programs, and graded motor exercises are introduced during rehabilitation to maximize the return of function. In some cases, secondary procedures (for example, tendon transfers or scar revisions) are planned to refine function once circulation and sensation have stabilized. Patients should expect progressive improvement over months to years, with the pace influenced by nerve gap length, patient age, and adherence to therapy.
What Are the Success Rates and Risks of Hand Replantation Surgery?
At North Texas Hand Center, P.A., we believe it is important for you to understand typical success rates and the potential risks when considering replantation surgery.
Advances in microvascular surgery have improved replantation viability, and published survival rates reflect these gains.
Survival of the replanted part (short-term viability) is one metric; long-term functional outcomes are another. Counseling before surgery covers both vascular success and realistic expectations for strength, range of motion, sensation, and the possible need for staged procedures and prolonged rehabilitation. Shared decision-making helps align surgical goals with your priorities—whether restoring length, preserving appearance, or maximizing useful function.
What Factors Affect the Success Rate of Finger and Hand Replantation?
Several factors influence replantation success, including:
- Timing of Surgery: Prompt surgical intervention is critical; the sooner the replantation occurs, the higher the chances of success.
- Patient Health and Age: Overall health and age can impact healing and recovery.
- Type of Injury: The nature and severity of the injury play a significant role in determining outcomes.
Our surgeons and you should weigh these factors carefully when assessing the likelihood of successful replantation.
Research further stresses that optimal results require comprehensive tissue repair and functional restoration, not only successful vascular reconnection.
Patient factors such as smoking, poorly controlled diabetes, or vascular disease can increase complication rates. Preoperative optimization—smoking cessation, glucose control, and addressing comorbidities—may improve the odds of both survival and functional recovery. Equally important is realistic goal setting: for some injuries, replantation may preserve a finger but not restore near-normal function, and alternatives (reconstruction, prosthesis) should be part of the discussion.
What Are the Potential Risks and Complications of Replantation Surgery?
Replantation carries risks. Common complications include:
- Infection Risks: Surgical sites can become infected, complicating recovery.
- Complications Related to Vascular and Nerve Repair: Issues such as blood clots or nerve damage can arise post-surgery.
- Long-term Management of Complications: Some patients may require additional surgeries or therapies to address complications.
Understanding these risks helps you make an informed decision about surgical options.
When complications occur, early recognition is key. For example, vascular compromise noticed in the early postoperative period may be reversible with return to the operating room for revision of anastomoses, exploration, or thrombectomy. Infection is managed with targeted antibiotics and, when necessary, additional debridement. Long-term problems such as cold intolerance, chronic pain, neuromas, stiffness, and scar tethering are addressed with a combination of therapy, medications, and sometimes secondary procedures.
How Is Recovery and Rehabilitation Managed After Hand Replantation?
Recovery and rehabilitation are central to long-term outcomes after replantation.
What Does Hand Microsurgery Recovery Involve?
Typical recovery after hand microsurgery includes:
- Initial Recovery Phase: Patients may experience swelling and pain, requiring careful management.
- Follow-up Care and Monitoring: Regular check-ups are essential to monitor healing and detect any complications early.
- Patient Education on Recovery: Understanding the recovery process helps patients set realistic expectations and engage in their care.
Careful recovery management is essential to help you achieve the best possible outcome.
Immediate postoperative management focuses on protecting vascular repairs, controlling pain, and preventing edema. Immobilization in a protective splint and elevation of the limb help support circulation. Our physicians commonly prescribe protocols for wound care, analgesia, and activity limitations. Anticoagulation or antiplatelet therapy may be used in selected cases following local protocols to reduce the risk of thrombosis in small-caliber vessels.
How Does Rehabilitation Therapy Improve Functional Outcomes?

Rehabilitation is key to regaining function after replantation. Important elements include:
- Types of Rehabilitation Therapies: Occupational and physical therapy can help restore movement and strength.
- Goals of Rehabilitation: The primary aim is to regain as much function as possible and improve the quality of life.
- Patient Success Stories: Many patients report significant improvements in hand function through dedicated rehabilitation efforts.
Rehabilitation supports your return to daily activities and helps restore independence and hand function.
Rehabilitation usually progresses through phases. Early passive motion may protect repairs while minimizing stiffness. As healing permits, therapists introduce active motion, strengthening, and task-specific training tailored to your functional needs—self-care, work tasks, and leisure activities. Sensory re-education and desensitization techniques address altered sensation and discomfort. Custom splints and adaptive equipment support functional gains while protecting healed repairs. The rehabilitation plan is individualized, typically involving frequent therapy visits in the first months and less frequent follow-up as you progress.
Psychosocial support is also important: traumatic amputations affect identity, independence, and mood. Counseling, peer support groups, and vocational rehabilitation help patients adapt and set realistic goals for return to work or daily roles.
What Are the Available Amputation Surgery Options and Alternatives?
When you face severe hand injury, it is important to understand the surgical options and alternatives available to you.
When Is Amputation Surgery Recommended Over Replantation?
Amputation may be advised in cases such as:
- Severe Tissue Damage: When the hand is beyond repair, amputation may be the best option.
- Infection Risks: If there is a high risk of infection that cannot be managed, amputation may be necessary.
- Patient Health Considerations: Overall health and the potential for recovery can influence the decision.
These factors help guide the decision toward the most appropriate surgical intervention for your situation.
When amputation is selected, our surgeons and therapists plan reconstruction and prosthetic strategies early. Partial amputation with good soft-tissue coverage may allow better prosthetic fitting and improved function compared with a less-planned approach. Shared planning with prosthetists, occupational therapists, and surgeons optimizes residual limb shape, scar placement, and preservation of useful joints.
What Are Prosthetic and Reconstructive Options After Amputation?
After amputation, several reconstructive and prosthetic options exist:
- Prosthetic Devices: Modern prosthetics can provide functional and aesthetic benefits, allowing for improved quality of life.
- Reconstructive Surgery: In some cases, reconstructive surgery may be an option to enhance appearance and function.
- Patient Adaptation and Support: Support systems and rehabilitation can help patients adjust to life after amputation.
These options can help you regain function and improve quality of life after amputation.
Prosthetic planning is multidisciplinary. Prosthetists evaluate residual limb shape and functional goals to recommend devices ranging from passive cosmetic fingers to body-powered or myoelectric systems for more complex tasks. Timing of prosthetic fitting depends on wound healing, scar maturation, and patient readiness. Reconstructive options such as toe-to-thumb transfers or local flap reconstructions are specialized procedures that may be appropriate in selected cases and are discussed within a comprehensive treatment plan.
How Can You Prepare for Hand Trauma Surgery and Schedule a Consultation?
Preparing for hand trauma surgery means understanding the process and what to expect during consultations.
What Should You Expect During Your Surgical Consultation?
At your surgical consultation with North Texas Hand Center, P.A., you can expect:
- Review of Medical History: A thorough assessment of your medical background is essential.
- Discussion of Surgical Options: Our surgeons will explain the available options and their implications.
- Preparation for the Consultation: We encourage you to come prepared with questions and concerns to discuss.
Bringing questions and discussing concerns helps you be informed and prepared for the treatment process.
During the consultation, our surgeons typically review imaging, discuss anesthesia options, outline expected hospital stay and rehabilitation, and explain potential complications. Ask about our surgical team’s experience with replantation, the expected postoperative therapy plan, and the timeline for follow-up. If possible, bring a family member or support person to help remember details and support decision-making.
How to Schedule Your Hand Replantation Surgery at North Texas Hand Center, P.A.?
To schedule surgery at North Texas Hand Center, P.A., follow these steps:
- Contact Methods for Scheduling: Reach out via our website or contact form to initiate the scheduling process.
- Required Documentation: You may need to provide medical records and insurance information.
- Insurance and Medical Clearance: Ensuring that all necessary approvals are in place is crucial for a smooth process.
Following these steps helps you prepare for surgery and secure the care you need.
Practical tips for scheduling and preparation include arranging transportation and post-discharge care, bringing pertinent medical records and a list of medications, and confirming any fasting or preoperative testing required by our surgical team. If the injury is emergent, our center’s triage and trauma protocols determine next steps; for elective reconstructions, coordinate appointments for preoperative clearance with your primary care and any specialists needed to optimize health before surgery.
After scheduling, ask our clinic for written instructions about preoperative medications, smoking cessation guidance, and contact information for questions. Early planning for rehabilitation appointments and prosthetic consultations shortens the time between surgery and functional recovery.
Schedule Your Consultation with North Texas Hand Center, P.A.
Understanding hand amputation and replantation surgery helps you make informed decisions about treatment and recovery. Timely intervention, advanced microsurgical techniques, and comprehensive rehabilitation contribute to better outcomes. We invite you to contact our expert team today for personalized guidance and to schedule a consultation.
Every injury and patient circumstance is unique. Our coordinated team approach—surgeons, therapists, prosthetists, primary care providers, and psychosocial supports—gives you the best chance to meet your goals. If you or a loved one is facing hand trauma, early contact with our experienced specialists preserves treatment options and supports an individualized path to recovery.